|
| Section 2 - Applied Pharmacokinetics |
Introduction
The aminoglycosides are the mainstay in the treatment of serious
gram-negative systemic infections. A disadvantage of the
aminoglycosides is their association with nephrotoxicity and
ototoxicity, both of which are associated with elevated trough
levels and sustained elevated peak levels.
Antimicrobial spectrum
Aminoglycosides are active against most strains of Staphylococcus
aureus and S. epidermidis. Most strains of enterococcus
are resistant to aminoglycosides alone, however when used in combination
with penicillins they are often effective in enterococcal endocarditis
due to synergistic antimicrobial mechanisms. Anaerobic bacteria are
universally resistant because aminoglycoside transport into cells is
oxygen-dependent.
Aminoglycosides have bactericidal activity against most gram-negative
bacteria including Acinetobacter, Citrobacter, Enterobacter, E. Coli,
Klebsiella, Proteus, Providencia, Pseudomanas, Salmonella, Serratia
and Shigella. The MIC's of gram negative bacteria are usually less
than 2 mcg/ml for gentamicin and tobramycin and 8 mcg/ml for amikacin.
Pharmacokinetics
When given by IV infusion over 30 minutes, aminoglycosides follow a 3-compartment
pharmacokinetic model; alpha (distribution), ß (elimination), and gamma
(tissue release). When infused over one hour, the distribution phase is usually
not observed. The gamma phase begins approximately sixteen hours post infusion,
drug that was tissue bound to various organs is released. The amount released
from tissue is very small, but does accumulate over time, contributing to AG toxicity.
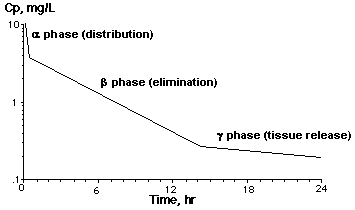
However, it is important to keep the true picture in mind when evaluating serum level data.
Concentration-toxicity relationships
Aminoglycosides can cause permanent vestibular and auditory ototoxicity.
Overt otoxicity generally occurs in 2% to 10% of patients treated with
aminoglycosides. Factors associated with otoxicity include duration of therapy,
elevated peak and trough levels, concurrent ototoxic drugs (loop diuretics),
underlying disease states, and previous exposure to aminoglycosides.
Vestibulotoxicity is difficult to diagnose and there is no reliable monitoring
process. Recent studies indicate a genetic predisposition to aminoglycoside
ototoxicity due to a mutation found in mitochondrial DNA.
Gentamicin toxicity is the most common single known cause of bilateral
vestibulopathy, accounting for 15-50% of all cases.
A web site, Wobblers Anonymous
presents personal testimony from patients who have suffered from this disabling ADE.
For gentamicin, tobramycin and netilmicin risk of ototoxicity and
nephrotoxicity is increased if trough levels consistently exceed 2 mcg/ml.
For amikacin, trough levels consistently greater than 10 mcg/ml have been
associated with a higher risk of ototoxicity and nephrotoxicity.
The reported incidence of nephrotoxicity varies substantially between
studies, averaging 6% to 10%. Nephrotoxicity rates do not vary significantly
among the different aminoglycosides. Factors associated with nephrotoxicity
include duration of treatment, increasing age, compromised renal function, volume
depletion, elevated peak and trough levels, concurrent nephrotoxic drugs (NSAIDs,
loop diuretics, Vancomycin)and previous exposure to aminoglycosides.
Concentration-efficacy relationships
Aminoglycosides eliminate bacteria quickest when their concentration is
appreciably above the MIC for an organism, this is referred to as concentration
dependent activity. The aminoglycosides also exhibit a significant post-antibiotic
effect (PAE). PAE is the persistent suppression of bacterial growth following
antibiotic exposure. Practically speaking this means that trough levels can drop
below the MIC of targeted bacteria for a sustained period without decreasing efficacy.
For AG's the ideal dosing regimen would maximize concentration, because
the higher the concentration, the more extensive and the faster is the degree
of bactericide. Therefore, the Peak/MIC ratio is an important predictor of efficacy.
It has been shown that aminoglycosides eradicate bacteria best when they achieve
a Peak/MIC ratio of at least 8-10. Therefore it is important to give a large enough
dose to produce a peak level 8 to 10 times greater than the MIC.
The pharmacodynamic properties of aminoglycosides are:
| Initial serum peak level | Died | Survived |
| < 5mcg/ml | 21% | 79% |
| >= 5mcg/ml | 2% | 98% |
Dosing methods
Dosage regimens necessary to achieve therapeutic aminoglycoside
serum concentrations can be quantitatively determined by using
simple pharmacokinetic principles. Individualized pharmacokinetic
parameters are determined from the patient's serum concentration
versus time data. Sawchuk and Zaske have described a method for
establishing multiple infusion regimens based on individually
calculated pharmacokinetic parameters. Lesar, et al found that
this individualized method achieved therapeutic concentrations
in 90% of patients.
For evaluation of serum level data, methods incorporating Bayesian
principles appear to give the best overall predictive performance
compared with traditional methods of vancomycin dosage adjustment.
The Bayesian approach combines both population and patient-specific
information (i.e., serum level data) in predicting dosage requirements.
Extended-interval (or "once-daily") aminoglycoside dosing has gained popularity
in recent years. The pharmacodynamic properties of AG's form the basis of EI dosing.
The concentration dependent activity of AG's demonstrates that a large dose (5mg/kg)
is needed to maximize killing. The persistent (post-antibiotic) effect of AG's allows
a dosing interval of 24-36 hours. This extended interval provides a beneficial wash
out period during the gamma (tissue-release) phase, thus decreasing the incidence of
toxicity.
This simplified dosing method is appropriate in young, otherwise healthy patients with sepsis.
However, there are many patients who are not candidates for the Extended-interval
dosing methodology, including those with the following conditions:
Achieving therapeutic serum levels of aminoglycosides early in the
course of treatment is critical to therapeutic success. Dosing error
on the high side is preferable to the risks of under-treatment. An
adequate loading dose is critical for rapid attainment of therapeutic
peak levels.
The method of Sarrubi and Hull utilizes serum creatinine,
lean body weight, age, and sex to estimate creatinine clearance.
This method considers more patient variables, which may improve
the estimation of aminoglycoside elimination. Lesar et al found
that the Sarubbi and Hull nomogram achieved therapeutic concentrations
in 78% of patients. Tsubaki and Chandler evaluated 5 methods
for determining initial dosing requirements for gentamicin. They
concluded that the Sarubbi and Hull method was the most accurate.
However, dosing nomograms are initial guidelines only. They
can produce substantial variations in serum concentrations and
should be subsequently adjusted based on serum level determinations
and clinical response.
Population model parameters
Elimination rate
Volume of distribution
The average Vd of AG's in otherwise healthy adults is 0.26 L/kg (range: 0.2-0.3).
Although AG's do not distribute into adipose tissue, they do enter the extracellular
fluid contained therein. Therefore, obese patients require a correction in the weight
used for Vd calculation: LBW + 40% of weight above LBW. Patients with cystic fibrosis
have a markedly increased Vd of 0.35 L/kg due to increases in extracellular fluid
brought about by the disease process. Patients with ascites have additional
extracellular fluid because of accumulation of ascitic fluid, which increases the
Vd to approximately 0.32 L/kg. Also, ICU patients may have a Vd 25-50% above normal.
AG elimination exhibits a close linear correlation with creatinine clearance, the
average value for slope is between 0.0024 and 0.0029 and y-intercept of 0.01 to 0.015.
Cystic fibrosis patients show a 50% increase in elimination rate. A major
body burn increases the basal metabolic rate resulting in a marked increase in
AG elimination. ICU patients are often hypermetabolic and therefore eliminate
AG's more rapidly.
| It is not possible to predict the exact effect a disease state will have on drug elimination, therefore, these special populations require intensive monitoring, usually on a daily basis. |
Monitoring parameters
Careful observation for signs of drug toxicity is imperative.
Obtain levels 24 hours after initiating therapy,
at steady state (approximately four half-lives), and every
2 to 3 days.
Measure every two days, or every day in unstable
renal function.
Weigh patient every two to seven days.
Measure and monitor urine output daily
Below are some general guidelines, however, target serum concentrations should
be individualized.
Peak
Serious infection: 6-8
Trough
Life-Threatening infection: 8-10
Serious infection: 0.5-1.5
Life-Threatening infection: 1- <2
Peak
Serious infection: 20-25
Trough
Life-Threatening infection: 25-30
Serious infection: 1-4
Life-Threatening infection: 4-8
Precautions
Drawing at exactly the right time is not as important as having the
lab note the exact times that the samples were drawn. Also,
have the nurse note the exact times that the sample infusion
was started and when it ended. Please be aware of the widespread
policy of nursing personnel to record a dose as having been given
exactly as ordered if it is given within 30 minutes of the recorded
time. This will lead to significant errors in analysis, please ensure
that all those involved record the exact times.
This issue cannot be stressed enough. Inaccurate recording of drug
administration times and lab draw times are the greatest source of
calculation error, having a greater effect than pharmacy preparation
error or lab assay error.
The trough sample should be obtained 30 minutes prior to the dose.
Measure the peak level 15 to 30 minutes after completion of the IV
infusion to avoid the distributive phase. Measure the peak level 90
minutes after an IM injection. Drawing the peak too soon will result
in inaccurate analysis.
In general the Bayesian approach to the determination of individual drug-dosage
requirements performs better than other methods. However, outlying patients
in a population (ie, those patients whose pharmacokinetic parameters lie outside
of the 95th percentile of the population) may be put at risk. As is always the case,
computerized algorithms can only assist in the decision-making process and should
never become a substitute for informed clinical judgement.
![]()
![]()
![]()
![]()
![]()
![]()
Section 2 - Applied Pharmacokinetics
www.rxkinetics.com
©Copyright 1984 - 2022, All rights reserved.
RxKinetics, Plattsburg, MO 64477